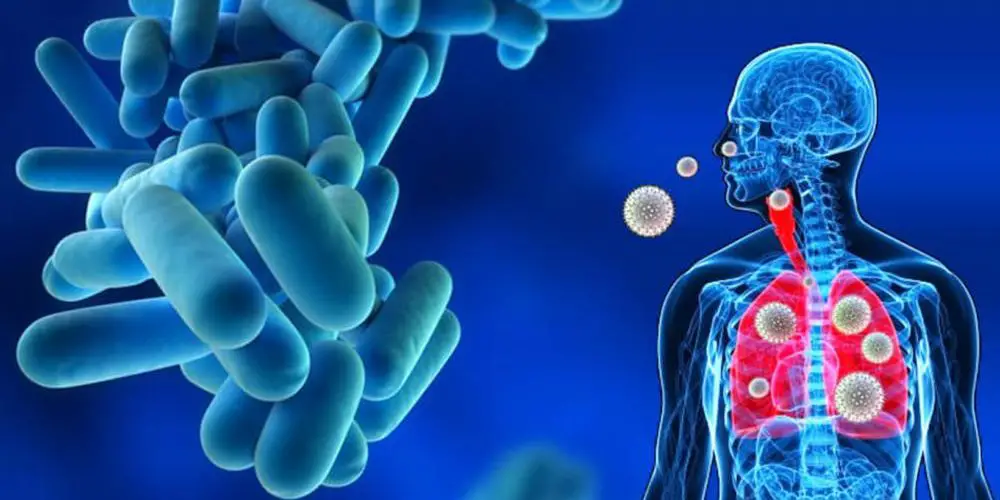
Legionellosis is a severe infectious disease characterized by general intoxication, damage to the respiratory, urinary and central nervous systems. Legionella is transmitted by aerosol. They are stable and can spread through cooling systems and compressors, in showers and swimming pools. As a rule, legionellosis is manifested by severe pneumonia with shortness of breath, chest pain and mucopurulent sputum. The diagnosis of legionellosis is established according to the data of sputum or bronchial flushing. Treatment is primarily antibacterial – antibiotics (erythromycin, rifampicin, pefloxacin).
General information
The causative agent of infection is mobile gram–negative anaerobes of the genus Legionella. For humans, 22 of the known 40 legionella species are dangerous. Bacteria secrete endotoxin, as well as a potent exotoxin. Legionella is stable in the environment, able to persist up to 112 days in water at a temperature of 25 ° C and 150 days at 4 ° C. The reservoir and source of infection are freshwater reservoirs (mainly with standing water) and soil. Legionella actively multiply in protozoa (for example, amoebas) at a temperature of 35-40 ° C, protecting themselves from the effects of chemical disinfectants, chlorine.
Due to their considerable adaptability, legionella often inhabit cooling systems, cooling towers, compressors, showers and swimming pools, as well as bathrooms for balneotherapy, installations for respiratory physiotherapy procedures, fountains. Often, the breeding conditions in artificial structures for legionella are more acceptable than in natural objects. A person is not a source of infection, even close contact with a patient does not lead to infection with legionellosis. Other animals or birds do not spread the infection either.
Legionellosis spreads by an aerosol mechanism, infection occurs when inhaling an air-water suspension containing bacteria. Epidemic outbreaks of legionellosis are often associated with the colonization of water cooling systems by bacteria, as well as with production cycles associated with the formation of fine aerosol. The pathogen can accumulate in air conditioners, shower cabins, dissipating in the air when turned on. When carrying out construction work, it is possible to implement an air-dust path of infection. Infection in medical institutions can occur during the passage of various procedures: vortex baths, the use of ultrasonic disintegrators, intubation, etc.
People have a high susceptibility to infection, its development is facilitated by smoking and alcohol abuse, as well as many chronic diseases: immunodeficiency conditions, lung diseases and metabolic disorders. The duration of immunity formed after infection is not known, but the disease does not occur again. Legionellosis is not uncommon among hotel clients, health workers and patients in geriatric or psychiatric hospitals. Mostly elderly people get sick, more often (more than 2 times) men.
Symptoms
The incubation period varies depending on the clinical form of infection, in general it can be 2 to 10 days. Its average duration is 4-7 days. In most cases, legionellosis occurs in the form of severe pneumonia (it is called “legionnaires’ disease”). Some patients have a prodromal period – there is a headache, weakness, loss of appetite, sometimes diarrhea. In other cases, the disease begins acutely, with a sharp rise in body temperature to high numbers and an increase in intoxication (chills, headaches, myalgia and arthralgia, sweating).
Soon intoxication affects the central nervous system, there is inhibition, emotional instability, delirium, hallucinations, fainting, impaired consciousness. Neurodisfunctions may occur – paralysis of the oculomotor muscles, nystagmus, dysarthria and ataxia. On the 3-4 day of the disease, a cough is detected, initially dry, subsequently with the separation of scanty mucopurulent (sometimes bloody) sputum. Shortness of breath and chest pain are characteristic (especially in the case of fibrous pleurisy). With auscultation in the lungs, wheezing (both dry and fine–bubbled), foci of respiratory weakness, with pleurisy – pleural friction noise. Percussion – dulling of sound over the affected segments and lobes.
The disease is difficult, it is difficult to treat. It is often complicated by exudative pleurisy, abscesses, contributes to the development of infectious and toxic shock. Often, progressive respiratory failure becomes an indication for transferring the patient to artificial ventilation. Cardiovascular disorders are the result of severe intoxication and general hypoxia due to developing respiratory failure.
Patients have arterial hypotension, rhythm disturbances (bradycardia is replaced by tachycardia). In a third of patients, the infection is accompanied by symptoms from the digestive system: diarrhea, abdominal pain, jaundice (accompanied by corresponding changes in the biochemical analysis of blood). Violations of urinary function up to acute renal failure can remain in the form of consequences for several months. Asthenic syndrome (weakness, fatigue, memory impairment) may persist for several weeks after infection.
Legionellosis can occur in the form of acute alveolitis. The disease also begins with increasing intoxication and fever, dry cough is present from the first days, later becoming wet, shortness of breath progresses. The alveoli sweat with fibrin and erythrocytes, the septa become edematous. In cases of prolonged progressive course of alveolitis, foci of pulmonary fibrosis are often formed.
Another form of legionellosis is Pontiac fever. In this case, the infection proceeds in the form of an acute respiratory disease. Intoxication is no less severe than in other forms, fever reaches 40 ° C, accompanied by rhinitis, inflammation of the upper respiratory tract. It is often accompanied by vomiting and abdominal pain, disorders of central nervous activity (insomnia, dizziness, impaired consciousness and coordination). In this form, the duration of the period of the main clinical manifestations usually does not exceed several days, the course of infection is benign. After the transfer of the disease, general asthenia also persists for some time.
Sometimes legionellosis occurs in the form of acute fever (Fort Bregg fever), accompanied by rashes of a diverse nature (roseolous, petechial, measles or scarlet fever-like exanthema). The rash does not have a localization specific to this infection and does not leave peeling after regression. In exceptional cases, there are other forms of legionellosis (generalized, septic, multiple organ).
Complications
It is extremely dangerous to complicate legionellosis with infectious and toxic shock, which often develops with legionellosis of the lungs. The mortality of patients in these cases can reach 20% of cases. In addition, due to the severity of the course, legionellosis can be complicated by multiple organ failures: cardiac, pulmonary, renal, hemorrhagic symptoms.
Diagnostics
A general blood test shows a picture of acute nonspecific bacterial infection (neutrophilic leukocytosis with a shift of the leukocyte formula to the left, a pronounced increase in ESR). General diagnostic measures (general and biochemical analysis of blood and urine) are carried out in order to monitor the state of organs and systems in the dynamics of the disease. In legionella pneumonia, lung radiography is informative, showing focal infiltrates in the lungs (lobar, subtotal or total pneumonia), as well as signs of pleurisy.
The pathogen is isolated by back-seeding from sputum, pleural fluid, flushing from the bronchi, noted in the blood. The most specific and accurate diagnostic method is bacteriological examination, but often, due to its complexity, they are limited to serological methods of RIF and ELISA. In addition, antibodies to legionella can be detected using RNIF and PMA. In the acute period of the disease, it is possible to isolate the pathogen antigen using ELISA and PCR.
Treatment
Etiotropic treatment of legionellosis consists in the appointment of macrolide antibiotics (erythromycin). In severe cases, the drug is prescribed intravenously by drip. Since legionella is quite difficult to respond to antibiotics, therapy is supplemented with rifampicin, the use of fluoroquinolones (pefloxacin) gives a good effect. The therapeutic course is usually up to 2-3 weeks.
Otherwise, the complex of therapeutic measures is aimed at reducing general intoxication, correcting respiratory failure, monitoring and treating disorders in the work of organs and systems. With the development of life-threatening complications, traditional intensive care measures are used. Patients with severe pneumonia are shown oxygenation, if indicated, transfer to artificial ventilation.
Forecast
About 15% of cases of the disease end in a fatal outcome, often this is due to the lack of timely medical care and the weakened general condition of the patients’ body. Concomitant chronic diseases, smoking, immunodeficiency increase the risk of an adverse outcome by 2-3 times. After the successful transfer of legionellosis, the consequences for the body are usually not noted, in rare cases, it is possible to preserve foci of fibrosis in the lungs (decreased breathing volume).
Prevention
Prevention of legionellosis consists in monitoring the condition of air conditioning and ventilation systems, bathrooms and shower cabins, devices for medical procedures. Disinfection methods for legionella are used both thermal (heating water to 80 ° C) and chemical (chlorine-based disinfectants). Flushing and cleaning of ventilation systems at enterprises and institutions (as well as in hotels) should be carried out at least 2 times a year. If legionella colonies are detected, the system is disinfected quarterly, followed by an epidemiological assessment of the water for the presence of the pathogen.
Currently, physical and chemical disinfection agents (ultraviolet irradiation, enrichment of water with silver and copper ions, chlorine-free compounds) are being actively introduced in order to reduce the damage caused by disinfection to ventilation and water supply systems. There is currently no specific prevention (vaccination) of legionellosis.